
5 Things I Wish Everyone with Osteoarthritis Knew as a Physical Therapist
If you’ve been diagnosed with osteoarthritis and immediately told a joint replacement is in your future- wow, I’m glad you’re here. This happens entirely too


If you’ve been diagnosed with osteoarthritis and immediately told a joint replacement is in your future- wow, I’m glad you’re here. This happens entirely too

One of the most debilitating consequences of shoulder arthritis is loss of range of motion. Shoulder arthritis exercises can be extremely effective in regaining motion

Hip pain when walking can limit the distance you’re able to go, the speed at which you can move as well as your enjoyment when

An arthritis specialist is someone who has experience in treating those with a certain type of arthritis, usually rheumatoid arthritis or osteoarthritis. These clinicians and
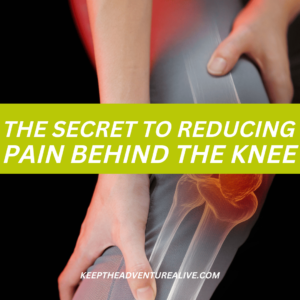
Tightness and pain in the back of the knee is a common issue that many people experience. It is also a common symptom of knee

Knee pain on stairs is not something you are doomed with when it comes to osteoarthritis. It is possible to regain strength, confidence and balance

When deciding on a joint replacement, consider reflecting on the severity of your pain, how your pain is affecting your social life and relationships, and

Climbing stairs will not make your osteoarthritis worse. Your cartilage actually loves when you move, so climbing stairs won’t cause more damage. Stairs could, though,

In order to prevent degenerative disc disease from getting worse, you have to understand why you’re in pain, find movements your body likes again, and
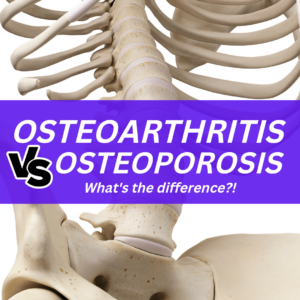
When trying to figure out the difference between osteoarthritis vs osteoporosis, they are actually more connected than you think. Osteoarthritis impacts the joints and osteoporosis

Copyright © 2023 Keep the Adventure Alive. All rights reserved.